By Francesco Giorgino
Diabetes mellitus describes a group of metabolic disorders characterized by chronically elevated glycemia. It represents one of the fastest-growing health challenges of the 21st century, with the number of adults living with diabetes having more than tripled over the past 20 years [1]. In particular, type 2 diabetes (T2D) accounts for 90% of all forms of diabetes and is caused by the loss of physiological beta-cell functional mass, responsible for inadequate insulin production and secretion, often concomitant to reduced insulin sensitivity in peripheral insulin-dependent tissues.
Extra virgin olive oil (EVOO) is a major component of the Mediterranean diet (MedDiet) and is appreciated worldwide because of its nutritional benefits in metabolic diseases, including type 2 diabetes (T2D) [2]. Indeed, the PREDIMED study showed that the consumption of MedDiet supplemented with EVOO determined a statistically significant 40% relative risk reduction of new-onset T2D compared to the control diet without EVOO [3,4]. Accordingly, lifestyle interventions, including the adoption of a healthy Mediterranean eating pattern, are effective and safe for improving glucose control in T2D and are recommended as firstline therapies from the time of diagnosis and as co-therapy for patients on glucose-lowering medications [5].
Although the high content of monounsaturated fatty acids was traditionally considered to be responsible for the beneficial effects of EVOO, recently, it has been suggested that most of the metabolic benefits of EVOO could be due to its minor components, particularly phenolic compounds (PCs) [2]. Accordingly, consuming EVOO rich in PCs for a total of 4 weeks improved metabolic control in T2D patients compared to the consumption of refined olive oil with no PCs [6].

Since the loss of beta-cell functional mass is a necessary and early condition in the development of T2D, and therefore beta-cell restoration or regeneration should be strongly considered for the treatment, and possible cure, of T2D [7], we investigated for the first time, simultaneously but individually, the effects of the main EVOO PCs on beta-cell function and survival.
We found that hydroxytyrosol, tyrosol, and apigenin foster beta-cell health by promoting proliferation and improving insulin biosynthesis (hydroxytyrosol, tyrosol, and apigenin), as well as by enhancing the insulin secretion (apigenin only). Interestingly, we also found that a mixture of hydroxytyrosol, tyrosol, and apigenin promotes the insulin secretion in human pancreatic islets. On the other hands, not all PCs showed a positive or neutral effect on beta-cell function and survival: some of them also induced cell death or reduced insulin secretion. These results suggest that only few PCs could be responsible for the anti-diabetes action of EVOO. Of note, to identify both the ideal EVOO PCs mixture against diabetes and the valid criteria to evaluate the real anti-diabetes potential of a specific EVOO, it is crucial to understand whether and to what extent each PC contributes to these beneficial metabolic effects.
In summary, in our study we have demonstrated that hydroxytyrosol, tyrosol, and apigenin, both alone and in combination, may preserve both function and survival of beta-cells, suggesting that EVOO or supplements enriched with these compounds may improve insulin secretion and promote glycemic control in T2D patients.
See article at https://www.mdpi.com/2223-7747/10/2/286

Prof. Francesco Giorgino, MD, PhD
President, Italian Society of Endocrinology (SIE)
Professor of Endocrinology
Chairman, Department of Emergency and Organ Transplantation
Head, Section of Internal Medicine, Endocrinology, Andrology and Metabolic Diseases
University of Bari Aldo Moro
Chief, Division of Endocrinology
University Hospital Policlinico Consorziale
Francesco Giorgino is Professor of Endocrinology and Metabolism and Chairman of the Department of Emergency and Organ Transplantation at the University of Bari Aldo Moro. He is also Chief of the Division of Endocrinology at the University Hospital Policlinico Consorziale, Bari, Italy.
Professor Giorgino received his medical degree from the University of Bari Aldo Moro and his PhD from the University of Naples Federico II, Italy. After completing his clinical and research training in endocrinology and metabolism at the University of Catania, Italy, he worked for several years at the Joslin Diabetes Center and Harvard Medical School, Boston, MA, USA, first as a postdoctoral research fellow and then as a visiting scientist.
Professor
Giorgino has received distinguished scientific awards from various
international and national institutions, including the Juvenile Diabetes
Research Foundation International Fellowship (New York, NY, USA), the Mary K.
Iacocca Foundation Fellowship (Boston, MA, USA), the Glaxo-Wellcome Award from
the European Association for the Study of Diabetes, the Aldo Pinchera and
Cassano Awards from the Italian Society of Endocrinology, and the Alcmeone
Award from the Italian Society of Diabetology. He has been the Italian delegate
in various European Commission Cooperation in Science and Technology actions
for diabetes research. Professor Giorgino has served on many national commissions
and national boards, including the Executive Committees and Scientific
Committees of the Italian Society of Diabetology and of the Italian Society of
Endocrinology.
He is currently President of the Italian Society of Endocrinology.
He is, or has been, an editorial board member for the following journals: PLoS
ONE, Journal of Endocrinology, Endocrinology, Journal
of Endocrinological Investigation, Adipocyte, Acta
Diabetologica, Cardiorenal Medicine, and Diabetes/Metabolism
Research and Reviews. He has published more than 200 original and review
articles in prestigious scientific journals and has been an invited speaker at
many national and international meetings. Professor Giorgino’s research
interests include the mechanisms leading to insulin resistance and beta-cell
dysfunction in Type 2 diabetes with a particular focus on skeletal muscle
metabolism and organ cross-talk, inflammation and lipotoxicity, and the effects
of diabetes drugs on pancreatic islets and the cardiovascular system. He has
also been involved in several clinical trials investigating the effects of
glucose-lowering drugs in individuals with Type 2 diabetes. He has an H-index
of 59 and over 10,000 citations (Google Scholar).
References
- Cho, N.; Shaw, J.; Karuranga, S.; Huang, Y.; Fernandes, J.D.R.; Ohlrogge, A.; Malanda, B. IDF Diabetes Atlas: Global estimates of diabetes prevalence for 2017 and projections for 2045. Diabetes Res. Clin. Pr. 2018, 138, 271–281.
- Mazzocchi, A.; Leone, L.; Agostoni, C.; Pali-Schöll, I. The Secrets of the Mediterranean Diet. Does [Only] Olive Oil Matter? Nutrients 2019, 11, 2941.
- Salas-Salvadó, J.; Bulló, M.; Babio, N.; Martínez-González, M.Á.; Ibarrola-Jurado, N.; Basora, J.; Estruch, R.; Covas, M.I.; Corella, D.; Arós, F.; et al. Reduction in the Incidence of Type 2 Diabetes with the Mediterranean Diet: Results of the PREDIMED-Reus nutrition intervention randomized trial. Diabetes Care 2010, 34, 14–19.
- Salas-Salvadó, J.; Bulló, M.; Estruch, R.; Ros, E.; Covas, M.-I.; Ibarrola-Jurado, N.; Corella, D.; Arós, F.; Gómez-Gracia, E.; Ruiz-Gutiérrez, V.; et al. Prevention of Diabetes with Mediterranean Diets. Ann. Intern. Med. 2014, 160, 1–10.
- Davies, M.J.; D’Alessio, D.A.; Fradkin, J.; Kernan, W.N.; Mathieu, C.; Mingrone, G.; Rossing, P.; Tsapas, A.; Wexler, D.J.; Buse, J.B. Management of Hyperglycemia in Type 2 Diabetes, A Consensus Report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care 2018, 41, 2669–2701.
- Santangelo, C.; Filesi, C.; Varì, R.; Scazzocchio, B.; Filardi, T.; Fogliano, V.; D’Archivio, M.; Giovannini, C.; Lenzi, A.; Morano, S.; et al. Consumption of extra-virgin olive oil rich in phenolic compounds improves metabolic control in patients with type 2 diabetes mellitus: A possible involvement of reduced levels of circulating visfatin. J. Endocrinol. Investig. 2016, 39, 1295–1301.
- Marrano, N.; Biondi, G.; Cignarelli, A.; Perrini, S.; Laviola, L.; Giorgino, F.; Natalicchio, A. Functional loss of pancreatic islets in type 2 diabetes: How can we halt it? Metabolism 2020, 154304.

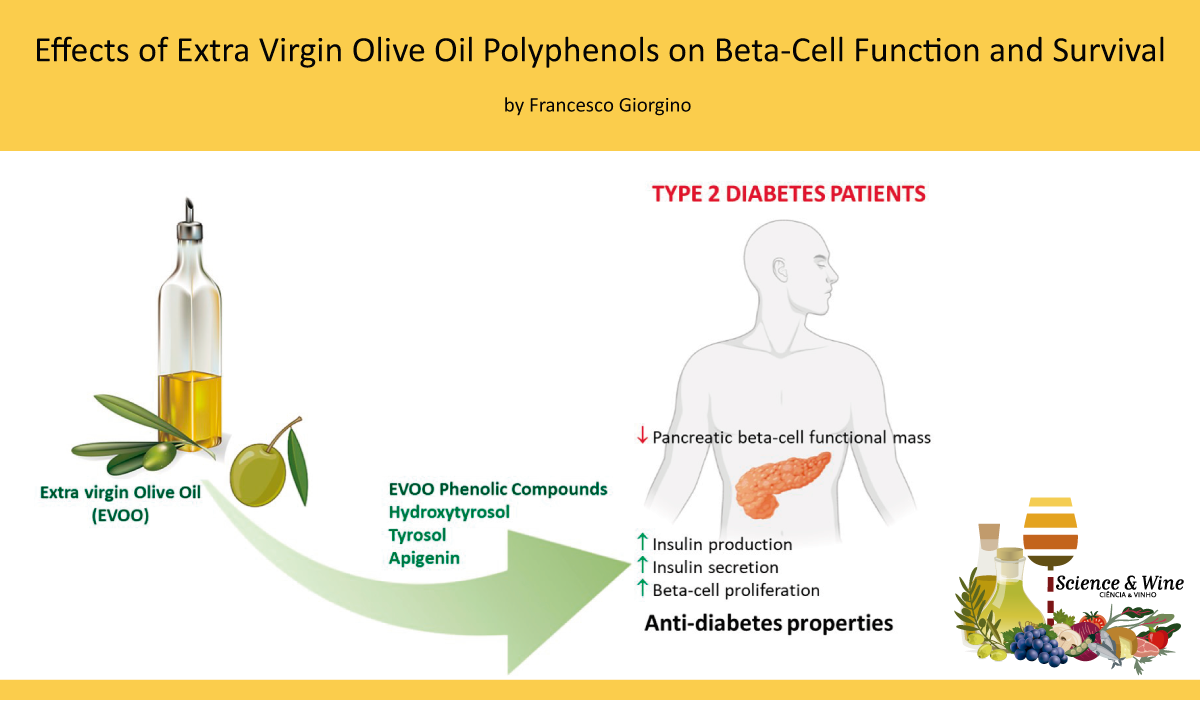
[…] Extra virgin olive oil (EVOO) is a major component of the Mediterranean diet and is appreciated worldwide because of its nutritional benefits in metabolic diseases, including type 2 diabetes (T2D). EVOO contains significant amounts of secondary metabolites, such as phenolic compounds (PCs), that may positively influence the metabolic status. This post reports a study where was investigated for the first time the effects of several PCs on beta-cell function and survival. The results show that hydroxytyrosol, tyrosol, and apigenin foster beta-cells’ health, suggesting that EVOO or supplements enriched with these compounds may improve insulin secretion and promote glycemic control in T2D patients. See all at: https://www.ciencia-e-vinho.com/2021/05/12/effects-of-extra-virgin-olive-oil-polyphenols-on-beta-cel… […]